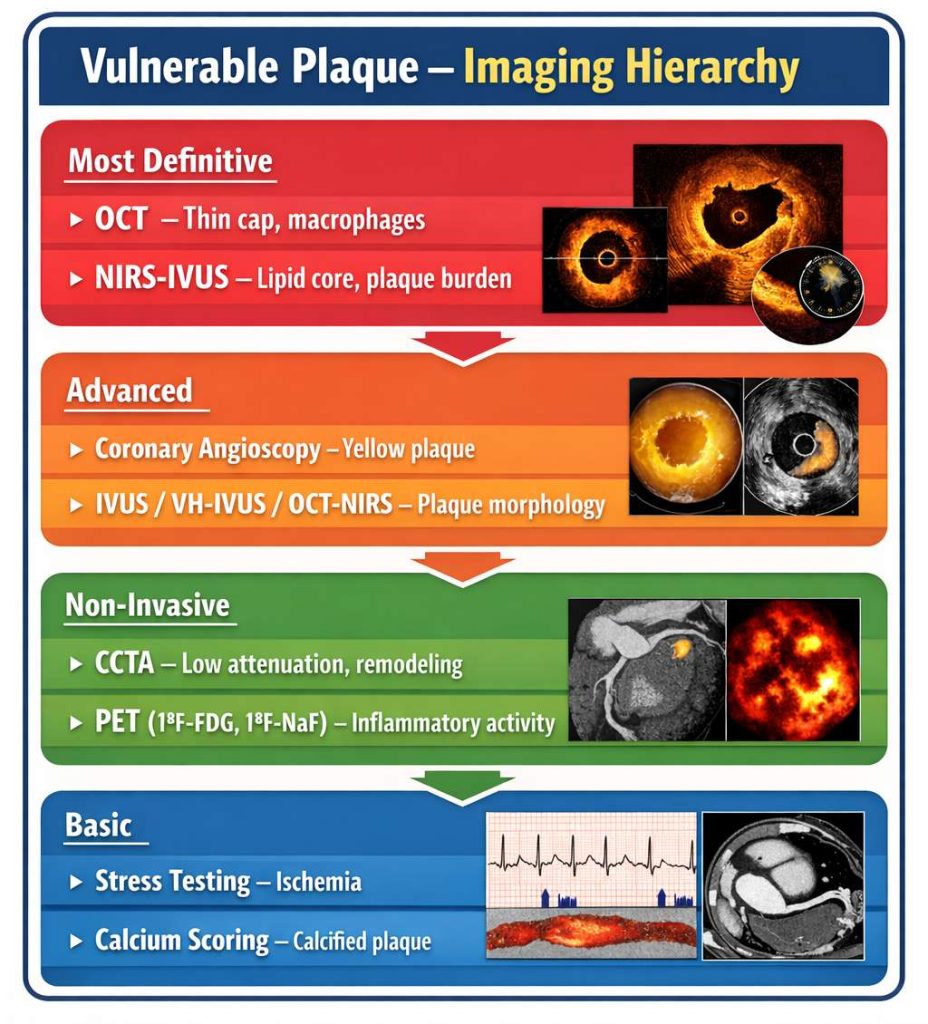
Methods to identify vulnerable plaque.
Vulnerable plaque = an atherosclerotic plaque prone to rupture or erosion, leading to ACS. Identification relies on morphology, composition, inflammation, biomechanics, and biology . No single modality is definitive; multimodal assessment is often required.
1. Invasive Coronary Imaging (Gold-standard for morphology)
1. Intravascular Ultrasound (IVUS)
Findings suggestive of vulnerability
Large plaque burden (>70%)
Positive (expansive) remodeling
Attenuated plaque (lipid-rich)
VH-IVUS : identifies thin-cap fibroatheroma (TCFA) patternLimit : poor cap thickness resolution
2. Optical Coherence Tomography (OCT) (Best for fibrous cap)
Highest axial resolution (~10–20 μm) Detects:
Thin fibrous cap (<65 μm) Lipid-rich plaque (lipid arc >90°)
Macrophage infiltration
Microchannels, plaque rupture, erosion
Current in-vivo gold standard for TCFA
3. Near-Infrared Spectroscopy (NIRS)
Quantifies lipid burden
Lipid Core Burden Index (LCBI)
LCBI >400 → high-risk plaque
Often combined with IVUS (NIRS–IVUS)
4. Coronary Angioscopy
Direct visualization
Yellow plaques = lipid-rich, vulnerableLimited availability; mainly research
2. Non-Invasive Coronary Imaging
5. Coronary CT Angiography (CCTA) (Most practical non-invasive tool) High-risk plaque features :
Low-attenuation plaque (<30 HU)
Positive remodeling
Napkin-ring sign
Spotty calcification
Clinical value : predicts future ACS independent of stenosis severity
6. Cardiac MRI (CMR)
Black-blood imaging for vessel wall
Identifies:
Lipid-rich necrotic core
Intraplaque hemorrhage
Limited spatial resolution for coronaries (better for carotids)
7. PET Imaging
18F-FDG → plaque inflammation (macrophages)18F-NaF → active microcalcification (rupture-prone)Hybrid PET–CT / PET–MRI improves localization
3. Functional & Biomechanical Assessment
8. Endothelial Dysfunction
Coronary vasomotor response to acetylcholine
Dysfunction correlates with plaque vulnerability
9. Hemodynamic Forces
Low endothelial shear stress (ESS) → plaque progressionHigh ESS at cap shoulders → rupture riskAssessed via computational flow dynamics (research)
4. Circulating Biomarkers (Adjunctive)
10. Inflammatory Biomarkers
hs-CRP
IL-6
MPO (myeloperoxidase)
11. Plaque Instability Markers
MMPs (matrix metalloproteinases)
Oxidized LDL
Lp-PLA₂
(Not plaque-specific; risk stratification only)
5. Emerging / Experimental Techniques
Molecular imaging of macrophages
Targeted nanoparticles
AI-based plaque phenotyping (CCTA + IVUS/OCT)
Radiomics for CT plaque texture
Exam-Oriented Summary (NEET-SS / DM Cardiology)
Modality Best Detects OCT Thin fibrous cap, macrophages (best overall) NIRS Lipid core burden IVUS Plaque burden, remodeling CCTA Non-invasive high-risk plaque features PET (NaF) Active microcalcification Angioscopy Yellow plaque
Key Point : Vulnerable plaque ≠ flow-limiting stenosis. Most ACS arise from mild–moderate lesions .
1. The single most specific in-vivo criterion for defining TCFA is:
A. Plaque burden >70%
B. Fibrous cap thickness <65 μm
C. Positive remodeling index >1.05
D. Lipid arc >90°
Only OCT-measured fibrous cap thickness <65 μm defines TCFA. Other features are supportive but non-definitive.
2. Which imaging modality has the highest spatial resolution for fibrous cap assessment?
A. IVUS
B. OCT
C. CCTA
D. PET-CT
OCT resolution is ~10–20 μm, far superior to IVUS (~100 μm).
3. Lipid Core Burden Index (LCBI) >400 is derived from:
A. OCT
B. NIRS
C. IVUS-VH
D. PET-NaF
NIRS quantifies lipid content and generates LCBI; >400 predicts future MACE.
4. Napkin-ring sign on CCTA represents:
A. Necrotic core surrounded by fibrous tissue
B. Dense concentric calcification
C. Thrombus over plaque rupture
D. Coronary spasm
Napkin-ring sign = low-attenuation core with peripheral higher attenuation rim → high-risk plaque.
5. Which PET tracer best identifies plaques prone to rupture rather than inflammation?
A. 18F-FDG
B. 18F-NaF
C. 13N-ammonia
D. Rubidium-82
18F-NaF binds to microcalcification, indicating active plaque destabilization.
6. A plaque causing ACS despite <50% stenosis most commonly represents:
A. TCFA with rupture
B. Stable fibrocalcific plaque
C. Chronic total occlusion
D. Isolated endothelial dysfunction
Most ACS arise from non-obstructive but vulnerable plaques.
7. Positive coronary remodeling on IVUS is defined as:
A. Plaque burden >70%
B. Remodeling index >1.05
C. Vessel area < reference
D. Presence of spotty calcification
Positive (expansive) remodeling = lesion EEM area ÷ reference EEM area >1.05, associated with vulnerable plaques.
8. OCT feature most specific for plaque erosion rather than rupture is:
A. Intact fibrous cap with luminal thrombus
B. Cap discontinuity
C. Large lipid arc
D. Macrophage clusters
Plaque erosion shows intact cap with overlying thrombus, unlike rupture where cap disruption is seen.
9. Which combination best defines a high-risk plaque on CCTA?
A. Dense calcification + negative remodeling
B. Low attenuation + positive remodeling
C. Long lesion length only
D. High calcium score alone
Low-attenuation plaque with positive remodeling is the classic vulnerable plaque phenotype on CCTA.
10. Attenuated plaque on IVUS typically represents:
A. Lipid-rich necrotic core
B. Dense calcium
C. Fibrous plaque
D. Organized thrombus
Attenuation without calcium shadowing on IVUS indicates lipid-rich vulnerable plaque.
11. Which modality directly visualizes plaque color?
A. Coronary angioscopy
B. OCT
C. IVUS
D. CCTA
Angioscopy shows yellow plaques, which correlate with lipid-rich vulnerable plaques.
12. Thin-cap fibroatheroma is MOST commonly detected in vivo by:
A. VH-IVUS
B. OCT
C. NIRS alone
D. CCTA
Only OCT can reliably measure fibrous cap thickness <65 μm in vivo.
13. Which plaque feature correlates BEST with inflammation?
A. Calcium arc >180°
B. Macrophage signal on OCT
C. Luminal stenosis severity
D. Lesion length
Macrophage infiltration reflects active inflammation and plaque instability.
14. Low endothelial shear stress is associated with:
A. Plaque progression and lipid accumulation
B. Cap rupture directly
C. Vessel spasm
D. Acute thrombosis alone
Low shear stress promotes plaque growth, while rupture often occurs at high shear regions.
15. Which PET tracer reflects macrophage metabolic activity?
A. 18F-FDG
B. 18F-NaF
C. 82Rb
D. 13N-ammonia
18F-FDG uptake reflects inflammatory macrophage activity in plaques.
16. Spotty calcification on CCTA suggests:
A. Active plaque instability
B. Plaque stabilization
C. Chronic healed plaque
D. Low-risk lesion
Small, spotty calcifications are associated with rupture-prone plaques.
17. Which OCT feature predicts future ACS independently?
A. Thin fibrous cap
B. Lumen area
C. Lesion length
D. Stenosis severity
Fibrous cap thickness is a stronger predictor than angiographic severity.
18. NIRS falsely underestimates lipid when:
A. Heavy calcium overlies lipid core
B. Plaque is superficial
C. Vessel is large
D. Positive remodeling exists
Calcium interferes with near-infrared signal penetration.
19. Plaque rupture most often occurs at:
A. Shoulder region of plaque
B. Center of necrotic core
C. Distal reference segment
D. Proximal normal vessel
High shear stress concentrates at plaque shoulders, predisposing to rupture.
20. Which biomarker best reflects plaque instability rather than burden?
A. Myeloperoxidase
B. LDL cholesterol
C. Total cholesterol
D. Triglycerides
MPO reflects oxidative stress and cap weakening.
21. In PROSPECT study, future events arose predominantly from lesions with:
A. Large plaque burden, mild stenosis
B. Severe angiographic stenosis
C. Normal IVUS
D. CTO lesions
PROSPECT showed non-obstructive plaques cause most future ACS.
22. Napkin-ring sign corresponds histologically to:
A. Necrotic core with thin fibrous rim
B. Pure fibrous plaque
C. Organized thrombus
D. Dense calcium
Peripheral higher attenuation reflects fibrous tissue surrounding lipid core.
23. Which is NOT a vulnerable plaque feature?
A. Thick fibrous cap
B. Lipid-rich core
C. Macrophage infiltration
D. Positive remodeling
A thick cap implies plaque stability.
24. Best modality to detect intraplaque hemorrhage is:
A. CMR
B. OCT
C. IVUS
D. Angioscopy
CMR is superior for detecting intraplaque hemorrhage, especially in carotids.
25. Which lesion is MOST likely to cause sudden ACS?
A. Mild stenosis with TCFA
B. 90% fibrotic stenosis
C. CTO
D. Calcified stable plaque
Vulnerability, not stenosis severity, determines ACS risk.
26. OCT overestimates lipid when plaque contains:
A. Large calcium shadow
B. Thin fibrous cap
C. Macrophages
D. Thrombus
Calcium causes signal attenuation mimicking lipid pools.
27. High-risk plaque progression is MOST associated with:
A. Low shear stress regions
B. High flow velocity
C. Turbulence only
D. Vasospasm
Low ESS promotes lipid accumulation and plaque growth.
28. Which combination best predicts plaque rupture?
A. Thin cap + large lipid core
B. Thick cap + calcium
C. Long lesion only
D. High-grade stenosis alone
Structural weakness plus lipid load defines rupture risk.
29. Which is TRUE regarding plaque erosion?
A. More common in younger patients and women
B. Always lipid-rich
C. Requires severe stenosis
D. Invisible on OCT
Plaque erosion often affects younger patients, smokers, and women.
30. Which imaging feature best correlates with future MACE?
A. TCFA on OCT
B. Angiographic stenosis
C. Vessel diameter
D. Lesion length
TCFA presence strongly predicts adverse events.
31. IVUS limitation in vulnerable plaque detection is:
A. Inability to measure cap thickness precisely
B. Poor penetration depth
C. Inability to assess remodeling
D. Radiation exposure
IVUS resolution is insufficient for thin fibrous cap measurement.
32. Which statement about vulnerable plaques is CORRECT?
A. They often cause ACS without severe stenosis
B. They are always heavily calcified
C. They are angiographically obvious
D. They rarely remodel positively
Most vulnerable plaques are angiographically mild.
33. Best non-invasive predictor of vulnerable plaque is:
A. CCTA plaque characteristics
B. Exercise ECG
C. Stress echo
D. Calcium score alone
CCTA allows direct plaque morphology assessment.
34. Which feature indicates plaque stabilization?
A. Thick fibrous cap with dense calcium
B. Spotty calcification
C. High lipid arc
D. Positive remodeling
Dense, confluent calcification is a marker of plaque healing.
35. Which combination is MOST dangerous?
A. High LCBI + thin cap
B. Low LCBI + thick cap
C. High calcium score alone
D. Long lesion without lipid
Lipid burden plus structural weakness defines maximal vulnerability.
36. Which modality best integrates structure and composition?
A. NIRS–IVUS
B. IVUS alone
C. OCT alone
D. Angiography
Hybrid NIRS–IVUS provides plaque burden and lipid composition.
37. Vulnerable plaque concept emphasizes:
A. Biology over luminal narrowing
B. Anatomy alone
C. Ischemia severity
D. Vessel size
Plaque composition and inflammation drive ACS risk.
38. Which statement regarding calcium is TRUE?
A. Microcalcification increases rupture risk
B. Dense calcium always causes ACS
C. Calcium score predicts culprit lesion
D. Calcium excludes vulnerability
Microcalcification causes local stress amplification, unlike dense calcium.
39. Ultimate clinical goal of vulnerable plaque detection is:
A. Prevent future ACS
B. Increase PCI rates
C. Detect all stenoses
D. Replace angiography
Identification aims at aggressive preventive therapy, not lesion counting.
40. The strongest predictor of future ACS among imaging features is:
A. Degree of luminal stenosis
B. Plaque vulnerability features
C. Coronary calcium score alone
D. Vessel diameter
Plaque composition and biology predict events better than stenosis severity.
Methods to identify vulnerable plaque Read More
Read More
Read More