A systematic approach to describing murmurs
A systematic approach to describing murmurs
When you hear a murmur, document its characteristics using the following parameters:
- Timing: Is it systolic, diastolic, or continuous?
- Shape: Does it increase in intensity (crescendo), decrease (decrescendo), or both (crescendo-decrescendo)? Or is it steady (plateau)?
- Location: Identify the valve area where the murmur is loudest.
- Aortic area: 2nd right intercostal space (ICS).
- Pulmonic area: 2nd left ICS.
- Tricuspid area: 4th left ICS.
- Mitral area: 5th left ICS at the midclavicular line (apex).
- Radiation: Does the sound spread to other areas, such as the axilla (mitral regurgitation) or the neck (aortic stenosis)?
- Intensity: Use the Levine grading scale, from Grade I (faint) to Grade VI (audible without a stethoscope). A palpable vibration, or “thrill,” is associated with a grade IV or higher murmur.
- Pitch and Quality: Descriptors can include high-pitched, low-pitched, blowing, harsh, or rumbling.
- Maneuvers: How do different positions or actions affect the sound?
- Handgrip: Increases afterload, strengthening murmurs like aortic regurgitation.
- Valsalva/Standing: Decreases preload, amplifying murmurs like those in hypertrophic cardiomyopathy.
- Squatting: Increases preload, amplifying most murmurs except hypertrophic cardiomyopathy.
Common murmurs for medical students
Systolic murmurs
- Aortic Stenosis (AS):
- Timing/Shape: Mid-systolic, crescendo-decrescendo.
- Location/Radiation: Loudest at the aortic area, radiates to the carotids.
- Other findings: A harsh quality, possibly a weak, slow-rising carotid pulse.
- Mitral Regurgitation (MR):
- Timing/Shape: Pansystolic (holosystolic), plateau.
- Location/Radiation: Loudest at the apex, radiates to the axilla.
- Other findings: A blowing quality, often requires the patient to be in the left lateral decubitus position to be best heard.
- Mitral Valve Prolapse (MVP):
- Timing/Shape: Mid-to-late systolic murmur preceded by a mid-systolic click.
- Location: Loudest at the apex.
- Maneuvers: Louder with Valsalva and standing.
- Ventricular Septal Defect (VSD):
- Timing/Shape: Pansystolic, high-pitched, and harsh.
- Location: Loudest at the tricuspid area.
- Note: The intensity is inversely proportional to the size of the defect; smaller holes create louder, harsher murmurs due to more turbulent flow.
Diastolic murmurs
- Aortic Regurgitation (AR):
- Timing/Shape: Early diastolic, decrescendo.
- Location/Radiation: Loudest at the left sternal border.
- Maneuvers: Best heard with the patient sitting up and leaning forward, holding their breath after exhalation.
- Mitral Stenosis (MS):
- Timing/Shape: Mid-diastolic, low-pitched, and rumbling.
- Location: Loudest at the apex.
- Maneuvers: Best heard with the bell of the stethoscope with the patient in the left lateral decubitus position.
How to use this information in clinical practice
- Start broad: Determine if the murmur is systolic, diastolic, or continuous by timing it with the carotid upstroke.
- Locate the sound: Find the point of maximum intensity to identify the likely affected valve.
- Refine your diagnosis: Use the other descriptive qualities—shape, pitch, quality, and radiation—to create a differential diagnosis.
- Perform maneuvers: Use simple maneuvers to confirm your hypothesis and strengthen your clinical picture.
- Refer for confirmation: Remember that your assessment is a clinical hypothesis. An echocardiogram is required for a definitive diagnosis.
Systematic Murmur Description
When you hear a murmur, approach it step by step using location, timing, intensity, pitch, quality, radiation, and maneuvers.
1️⃣ Timing (When does it occur?)
- Systolic (between S1 and S2)
- Ejection systolic (crescendo-decrescendo): Aortic stenosis, pulmonary stenosis
- Holosystolic/pansystolic (uniform): Mitral regurgitation, tricuspid regurgitation, VSD
- Late systolic: Mitral valve prolapse
- Diastolic (after S2, before S1)
- Early diastolic: Aortic regurgitation, pulmonary regurgitation
- Mid-diastolic: Mitral stenosis, tricuspid stenosis
- Late diastolic (presystolic): Mitral stenosis accentuated by atrial contraction
- Continuous (throughout systole and diastole)
- PDA, AV fistula, venous hum
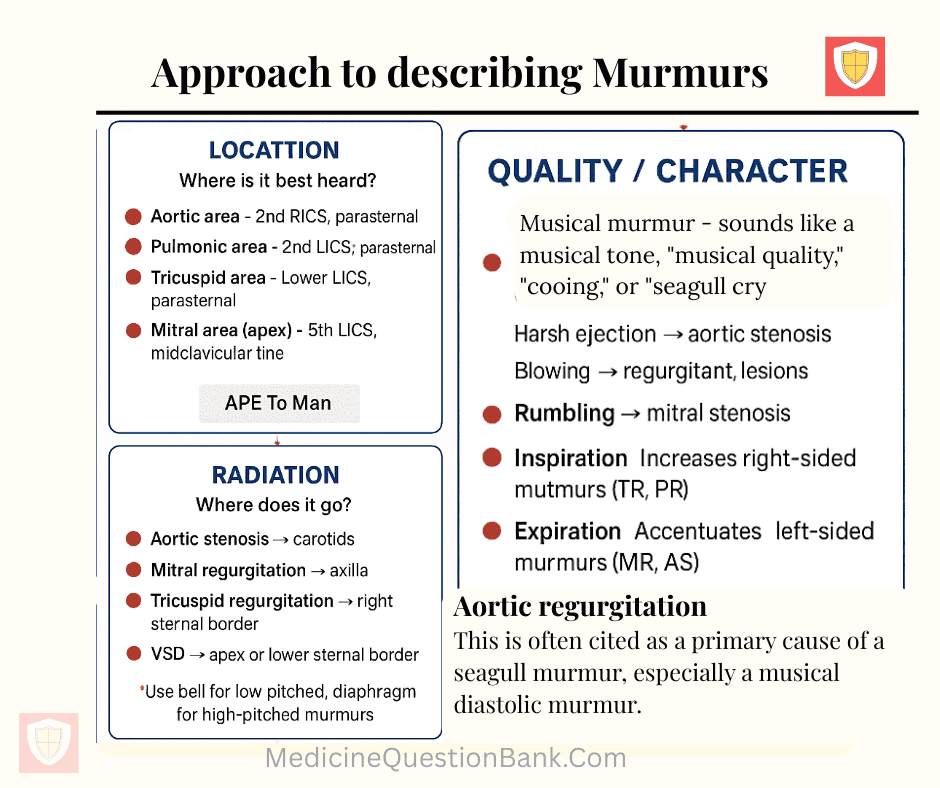
2️⃣ Location (Where is it best heard?)
- Aortic area: 2nd RICS (right 2nd intercostal space), parasternal
- Pulmonic area: 2nd LICS, parasternal
- Tricuspid area: Lower LICS, parasternal
- Mitral area (apex): 5th LICS, midclavicular line
Tip: “APE To Man” mnemonic: Aortic – Pulmonic – Tricuspid – Mitral
3️⃣ Radiation (Where does it go?)
- Aortic stenosis → carotids
- Mitral regurgitation → axilla
- Tricuspid regurgitation → right sternal border
- VSD → apex or lower sternal border
4️⃣ Intensity (Grade / Loudness)
Levine scale (I–VI):
- Barely audible
- Soft but audible
- Moderate, easy to hear
- Loud, with thrill
- Very loud, can hear with stethoscope partly off chest, thrill
- Audible with stethoscope off chest, thrill present
5️⃣ Pitch
- High-pitched: Mitral regurgitation, aortic regurgitation
- Medium: Aortic stenosis (usually ejection), pulmonic stenosis
- Low-pitched: Mitral stenosis, VSD (small), tricuspid stenosis
Use bell for low-pitched, diaphragm for high-pitched murmurs
6️⃣ Quality / Character
- Harsh / blowing / musical / rumbling / crescendo-decrescendo
- Examples:
- Harsh ejection → aortic stenosis
- Blowing → regurgitant lesions
- Rumbling → mitral stenosis
7️⃣ Shape / Configuration
- Crescendo: Increases in intensity
- Decrescendo: Decreases
- Crescendo-decrescendo: Ejection murmur
- Holosystolic / plateau: Uniform throughout systole
8️⃣ Maneuvers / Physiologic Changes
- Valsalva / standing: Decreases venous return, reduces most murmurs except HOCM, MVP (increase)
- Squatting / handgrip: Increases afterload; handgrip accentuates MR, AR, VSD; squatting decreases HOCM intensity
- Inspiration: Increases right-sided murmurs (TR, PR)
- Expiration: Accentuates left-sided murmurs (MR, AS)
9️⃣ Associated Findings
- Thrills, clicks (e.g., MVP), opening snaps (MS), S3/S4
- Signs of volume overload: pulmonary edema, jugular venous distension
10️⃣ Summary Table (Mnemonic: “T-RIM-P-Q”)
| Feature | Question to ask | Example |
|---|---|---|
| Timing | When? Systolic/Diastolic | Mid-systolic ejection |
| Radiation | Where does it go? | Carotids, axilla |
| Intensity | Grade 1–6 | 3/6 systolic |
| Mechanics / Maneuvers | Increases / decreases | Squatting accentuates AS |
| Pitch | High / low / medium | High-pitched blowing |
| Quality | Harsh / rumbling / musical | Harsh ejection |
| Location | Best heard | Aortic area |
✅ Clinical Tip: Always describe murmurs in this order:
Timing → Location → Radiation → Intensity → Pitch → Quality → Maneuvers → Associated findings
🩺 Systematic Approach to Describing Heart Murmurs — 20 MCQs
30 FAQs — Medical Students (General & Clinical)
Use short focused blocks (Pomodoro 25–50 min), alternate active learning (questions, flashcards) with passive review (notes), prioritize high-yield topics, and schedule weekly spaced repetition sessions.
Read abstract → conclusions → figures/tables → methods, then introduction. Critically appraise PICO, sample size, bias, outcomes, and clinical relevance.
Introduce yourself, confirm patient ID and consent, perform focused history/exam using a checklist, verbalize reasoning, summarize findings, and propose next steps. Time management is key.
Use lead groups: II, III, aVF → inferior; V1–V4 → anterior; V5–V6, I, aVL → lateral. Correlate with supplying coronary artery (RCA, LAD, LCx).
Follow the systematic approach: Timing → Location → Radiation → Intensity (grade I–VI) → Pitch → Quality → Maneuvers → Associated signs (S3/S4, click, snap).
Assess pH (acidosis/alkalosis), PaCO₂ (respiratory component), HCO₃⁻ (metabolic component). Determine primary disturbance and compensation; use anion gap to refine metabolic acidosis.
Start with clinical probability (Wells or Geneva). If low/moderate, a D-dimer; if positive or high probability, CT pulmonary angiography (CTPA). Consider V/Q scan if contraindications to CT.
Focus on drug classes, mechanisms, major side effects, and major contraindications. Use flashcards, compare similar drugs in tables, and practice clinical vignettes linking drugs to diseases.
Check if the expected compensation matches the measured values. If not, suspect mixed disorders. Use formulas (Winter’s, expected PaCO₂) and calculate anion gap and delta ratio for metabolic acidosis mixtures.
Use a stepwise method: rate → rhythm → axis → intervals → QRS morphology → ST/T changes → correlate clinically. Practice many strips and learn patterns (AF, flutter, blocks, STEMI territories).
Indicated for high-risk cardiac conditions (prosthetic valve, prior infective endocarditis, certain congenital heart disease) during dental or infected mucosal procedures — follow current guideline recommendations for agents/dosing.
Use a problem-oriented mini-presentation: 1-sentence summary (age, complaint, keyDx), brief HPI, salient exam, most relevant investigations, differential (top 3), plan and rationale.
Early recognition, blood cultures, broad-spectrum IV antibiotics within the first hour, fluid resuscitation (e.g., 30 mL/kg crystalloid if hypotensive), source control, and frequent reassessment.
Systematic review: AP/PA/LAT? Quality/rotation? Cardiomediastinal silhouette, lung fields (zones), pleural spaces, lines/devices, and look for common pathologies (consolidation, effusion, pneumothorax).
Listen for S1 and S2: systolic murmurs occur between S1 and S2; diastolic murmurs occur after S2 before S1. Use carotid pulse palpation — murmur that occurs with carotid upstroke is systolic.
“SNOOP” red flags: Systemic symptoms, Neurologic signs, Onset sudden (thunderclap), Older age/new onset, Previous cancer or immunosuppression — consider imaging/lumbar puncture.
Start with the most life-threatening and most likely conditions based on red flags and local epidemiology; use history clues to rule in/out quickly and choose targeted investigations.
Use narrowest effective agent, treat appropriate duration, avoid unnecessary broad-spectrum use, de-escalate based on cultures, and consider local resistance patterns.
Determine tonicity (hypotonic, isotonic, hypertonic), volume status (hypovolaemic, euvolaemic, hypervolaemic), and calculate urine sodium/osmolality to guide cause and treatment.
Use structured format (SBAR: Situation, Background, Assessment, Recommendation), highlight pending tasks, escalate unstable patients, and confirm recognition from receiver.
Anion gap = Na⁺ − (Cl⁻ + HCO₃⁻). Elevated gap suggests accumulation of unmeasured anions (e.g., lactic acidosis, DKA, toxins). Helps classify metabolic acidosis.
Suspect with fever, neck stiffness, altered mental status. Do blood cultures, give empiric IV antibiotics and dexamethasone promptly; perform CT head if focal signs or raised ICP before LP.
Practice concise explanations, understand core principles rather than rote facts, rehearse common scenarios aloud, and review exam-specific procedures and guidelines.
Iron deficiency, anaemia of chronic disease (less commonly microcytic), thalassaemia, and sideroblastic anaemia. Use ferritin, TIBC, and Hb electrophoresis to differentiate.
Explain diagnosis, proposed intervention, benefits, common and serious risks, alternatives (including no treatment), and check patient understanding and voluntary agreement; document the discussion.
Look at FEV₁/FVC ratio: reduced → obstructive (e.g., COPD, asthma). Reduced FVC with normal/high ratio → restrictive disease. Use bronchodilator response and lung volumes for further distinction.
Consider systemic causes (heart failure, liver disease, renal disease), local causes (venous insufficiency, lymphedema), medication-related, and assess pitting, distribution, and timing.
Plan a short prioritized task list each morning (3–5 items), do focused learning around patient care opportunities, and review short learning goals after rounds to consolidate knowledge.
Troponin detects myocardial injury — not specific to type I MI. Consider myocarditis, supply–demand mismatch (type II MI), renal failure, PE, and chronic structural disease. Correlate clinically and with ECG.
Use specific, behavior-focused feedback (what, impact, suggestion). Be timely, balanced, and invite reflection. As a receiver, listen actively, ask clarifying questions, and make a plan to improve.







